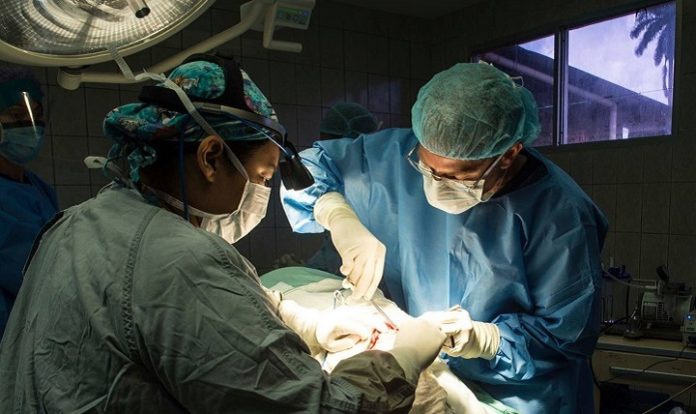
Two studies from the University of Texas MD Anderson Cancer Center show that abdominal hysterectomy has better outcomes for cervical cancer
Two studies led by researchers at The University of Texas MD Anderson Cancer Center discovered that minimally invasive radical hysterectomy is associated with higher recurrence rates and worse overall survival (OS), compared to abdominal radical hysterectomy in women with early-stage cervical cancer.
The results of both studies are published in the New England Journal of Medicine. The first, a randomized-controlled Phase III trial, was led by Pedro Ramirez, M.D., professor, Gynecologic Oncology and Reproductive Medicine. The second, an epidemiologic study, was led by J. Alejandro Rauh-Hain, M.D., assistant professor, Gynecologic Oncology and Reproductive Medicine and Health Services Research.
According to the authors, the findings already have changed care at MD Anderson and could impact the surgical management of all women with early-stage disease, which accounts for nearly half of the 13,240 cervical cancers expected to be diagnosed this year.
In India, cervical cancer is the second most common cancer among women. National health Profile data shows that in 2013, 92,731 cases of cervical cancer were reported in India, a figure that is projected to go up to 1,00,479 in 2020.
The rate of disease-free survival at 4.5 years was 86 percent with a minimally invasive surgery and 96.5 percent with open surgery
“Minimally invasive surgery was adopted as an alternative to open radical hysterectomy before high-quality evidence regarding its impact on survival was available,” said Rauh-Hain. “Both Dr. Ramirez and I were surprised to find that in our respective studies, surgical approach negatively affected oncologic outcomes for women with early-stage cervical cancer.”
In the gynecologic oncology community, minimally invasive surgery for cervical cancer gained acceptance more than a decade ago as an alternative to abdominal radical hysterectomy when laparoscopy and then robotic technology were introduced. However, impact on survival and other cancer-related outcomes had not been studied in randomized trials or large, well-designed observational studies.
“Until now, data focused primarily on surgical outcomes and the immediate period after, such as the recovery of the patient, length of stay, transfusion needs, and overall return to functional daily activities,” said Ramirez. “Our research is the first to prospectively compare the two surgical approaches and evaluate oncologic outcomes, including disease-free and overall survival and recurrence rates.”
The findings are critical, say the researchers, because cervical cancer is curable with surgery in its earliest stage but treatments are much less effective after disease recurrence.
Phase III clinical trial reports worse outcomes with minimally invasive hysterectomy
In their study, Ramirez and colleagues hypothesized that minimally-invasive radical hysterectomy was equivalent to the open approach in terms of disease-free survival (DFS). The international study was a multi-institutional collaboration with 33 centers worldwide.
The researchers found:
- Minimally invasive radical hysterectomy was associated with a three-fold increase in disease progression, compared to open radical hysterectomy.
- The rate of disease-free survival at 4.5 years was 86 percent with a minimally invasive surgery and 96.5 percent with open surgery.
- The three-year OS overall survival was 91.2 percent in the minimally invasive group compared to 97.1 percent in the open surgery arm.
“Our study reinforces the need for more randomized clinical trials in the field of surgery,” said Ramirez. “Too often, success of a new intervention in surgery is measured by retrospective data. We always need to test and measure our procedures to determine what is best for our patients.”
Retrospective study reinforces clinical trial findings
Rauh-Hain’s retrospective, epidemiologic study also confirmed that minimally invasive radical hysterectomy was associated with worse OS than abdominal radical hysterectomy among patients with early-stage cervical cancer. The study, performed in collaboration with Harvard, Columbia University, and Northwestern University, includes analysis of data from two large cancer databases to compare survival rates between patients who underwent either of the two surgery types.
The team first analyzed the National Cancer Database (NCDB); this nationwide outcomes registry covers approximately 70 percent of newly diagnosed cancer cases in over 1,500 U.S. hospitals. The secondary analysis reviewed data from the National Cancer Institute’s (NCI) Surveillance, Epidemiology and End Results (SEER) database.