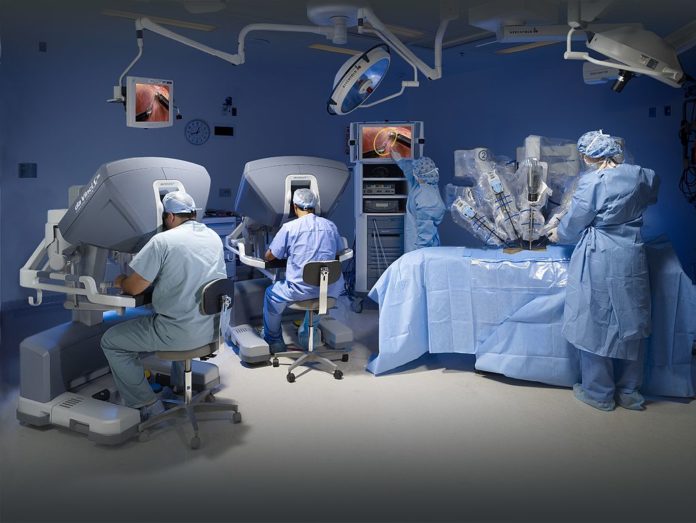
The plan to cap profit margins, offer discounts in case of deaths could deny patients the best possible care in the first 24 hours
That the temptation to resort to populist band aids for a broke health system cuts across party lines was proved yet again when Delhi government announced its plan to rein in reckless profiteering by the private sector.
The basic tenets of the policy to be incorporated in the Delhi Nursing Homes Registration Act after 30 days are – drugs under price control should be used as much as possible, a profit cap of 50% on drugs that are not under price control, 30% profit margin on implants and a discount on the bill in case the patient dies within 24 hours of hospitalisation. It neither attempts to fix the public-private divide in the health system, nor does it strike at the root of the malpractices in the private sector. All it does is that it gives the functionaries of the Aam Aadmi Party government a stick to beat the private sector with and beat its own drums in political speeches.
Since the 1990s India has pursued a policy geared towards privatisation of healthcare; it isn’t a certificate for the efficiency of the private sector but merely a realistic assessment of the severe limitations of the public health system. According to the report of the High-Level Expert Group (HLEG) formed by the erstwhile Planning Commission to look into how India could move towards universal health coverage, “From 8 per cent in 1947, the private sector now accounts for 93 per cent of all hospitals, 64 per cent of all beds, 80 per cent to 85 per cent of all doctors, 80 per cent of out-patients, and 57 per cent of in-patients.” Of the 1.37 million functional hospital beds in India, 8,33,000 are in the private sector.
Successive governments in both states and the Centre have to bear the responsibility for this abject surrender.
The AAP policy has not been thought through. For one – most private hospitals charge the MRP on drugs and consumables. The fact that MRP is inflated by pharmaceutical companies to push their own sales is the worst kept secret of the industry. The same Meropenem that is being sold at a private hospital at MRP will be sold at 30-50% less in select chemist shops in areas where the competition is stiff – for example Yusuf Sarai or Jamia Nagar in Delhi. What is the profit margin cap on? Is it on the markup on MRP or is it on the manufacturing cost? How does the Delhi government plan to regulate inflated MRPs?
This, when for many patients including those with trauma and stroke time is of great essence. A patient in other words may have to clear the 24 hour “uncertainty” period before treatment can effectively start.
One important perspective – prices of orthopaedic implants and cardiac stents were capped last year. Yet the cost of the procedures did not change. Why not a system of prescription audit? An audit that penalises repeat offender doctors for overprescription and other malpractices is an option that at least needs to be discussed.
The discount on Bills – 50% in caes of death within 6 hours and 20% for death within 24 hours of admission – is a far more dangerous proposition, not because private hospitals do not indulge in unethical practices but precisely because they do. It is possible for a patient to be denied crucial and expensive life saving interventions within the first 24 hours should the person be in a precarious position. Because if s/he does not make it, the hospital would have to waive a part of the Bill. This, when for many patients including those with trauma and stroke time is of great essence. A patient in other words may have to clear the 24 hour “uncertainty” period before treatment can effectively start.
The health system is in need of systemic reforms and governments have always shirked that role – perhaps because any effective systemic change would need considerable infusion of funds and not the least because financial muscle is very clearly on the other side. That any industry flush with funds can gently guide policy in that sector is not exactly a revelation. The one way to prevent the private sector from doing unnecessary tests to inflate bills is to have standard treatment guidelines. STGs for several conditions and disease are already in place but there is clearly no will to implement.
Last but not the least, abdication of healthcare responsibility to the private sector is also a cop out. Article 47 of the Directive Principles of State Policy lays down: “Duty of the State to raise the level of nutrition and the standard of living and to improve public health: The State shall regard the raising of the level of nutrition and the standard of living of its people and the improvement of public health as among its primary duties and, in particular, the State shall endeavour to bring about prohibition of the consumption except for medicinal purposes of intoxicating drinks and of drugs which are injurious to health.”
If states – and the Centre – had given half as much attention to that responsibility as they did to Article 48, private healthcare sector would not have become such a necessary evil that it now has, a Frankenstein monster that is out of control.
Article 48 lays down that prevention of cow slaughter is a state obligation.