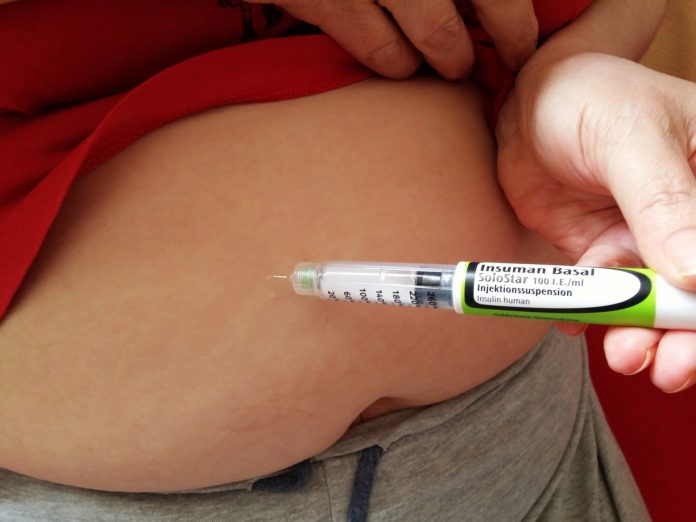
Patients underuse insulin so as to make it last longer
For patients with diabetes, insulin is a life-saving medicine and an essential component of diabetes management. Yet, in the past decade alone, the out-of-pocket costs for insulin have doubled in the United States.
One-quarter of patients with type 1 or 2 diabetes have reported using less insulin than prescribed due to these high costs, Yale researchers write in JAMA Internal Medicine. Over a third of those patients experiencing cost-related underuse said they never discussed this reality with their provider.
One in four respondents indicated they’d done at least one of those underuse behaviors in the past year due to insulin’s out-of-pocket cost
“You might have heard stories of patients rationing their insulin,” said Yale endocrinologist and senior author Dr. Kasia Lipska. “The stories are really powerful, but they don’t tell us how common this problem has become. Our findings show that these are not isolated incidents and that skimping on insulin is frighteningly common. As clinicians, we have to advocate for change because the status quo is simply cruel and not acceptable.”
Researchers surveyed a diverse sample of patients from across New Haven County, Connecticut, who use the Yale Diabetes Center for treatment. They asked patients about many different types of cost-related insulin underuse: using less insulin than prescribed, trying to stretch out one’s prescribed insulin, taking smaller doses of insulin than prescribed, stopping the use of insulin, not filling an insulin prescription, and/or not starting insulin.
One in four respondents indicated they’d done at least one of those underuse behaviors in the past year due to insulin’s out-of-pocket cost.
“The data we collected speak loud and clear to the fact that cost is a huge barrier to insulin accessibility,” said Pavithra Vijayakumar, co-first author and Yale medical student. “I hope this spurs more action to help patients afford this life-sustaining medication.”
The survey found that the quarter of patients who’d indicated they engaged in any type of insulin underuse were much more likely (43% versus 28%) to have poor glycemic control, an important indicator of the effectiveness of diabetes management. Additionally, they found that lower-income patients were more likely to report cost-related underuse, and nearly two-thirds of those patients reported that they also experienced difficulty affording other diabetes management equipment.
“It was really eye-opening to hear patients’ stories as they turned in completed surveys,” said Darby Herkert, co-first author of the study and Yale undergraduate. “I’ve worked in various global health settings, but this brought home to me how much patients struggle with costs right here in New Haven.”